- Traverse City, MI |
-
West: W Front St:
 (231) 944-6541
(231) 944-6541
-
| Central: Munson Ave :
 (231) 421-9300
(231) 421-9300
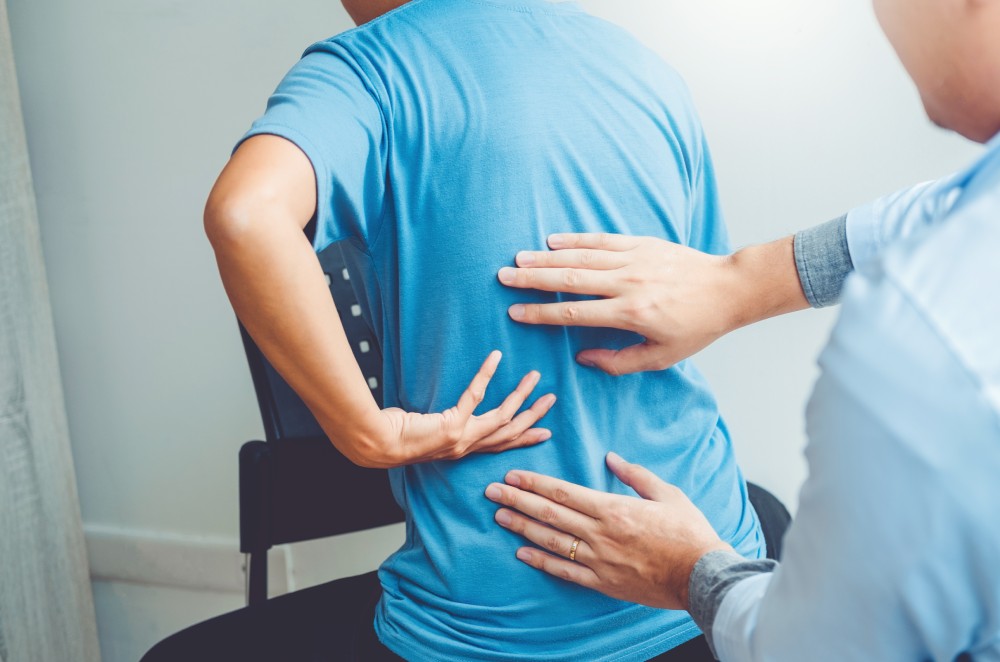
Disc herniation, also called slipped disc or ruptured disc, happens when a disc located between vertebrae in the spinal column is displaced.
It is one of the most common reasons for persistent pain in the lower back and leg region for adults. Disc herniation therapy is recommended for patients with this condition.
The discs mentioned here are the rubbery materials separating each vertebra. They act as shock absorbers when the spine is flexed, bent, or twisted. These discs have a soft, jellylike center called the nucleus which is surrounded by a rubbery exterior called the annulus.
Disc herniation occurs when parts of the nucleus seeps or pushes out of the annulus through a tear or a crack. This can happen in any part of the spinal column. When the herniation comes in contact with and irritates the nearby nerve, it can result in weakness, numbness, or pain radiating to the arm or leg.
We've got lots more info on the causes of back pain and how to heal on our BLOG.
Although most herniated discs occur in the lower back, they can still happen elsewhere in the spine up to the neck. The symptoms depend on where the disc is located and whether the herniation is affecting or pressing on a nearby nerve.
The following may serve as indications where the herniated disc is situated:
Pain, weakness, or numbness in the leg region, including the thigh, calf, buttocks, and, in some cases, even in the feet usually means that the herniated disc is located in the lower back or in the lumbar region.
Symptoms in the shoulders, arms, and hands generally point to a herniated disc near or on the neck area.
The numbness or tingling radiates to the extremities from the affected nerves in the spine. Additionally, weakness can also manifest in the muscles that are served by the affected nerves. These symptoms can cause a person to lose their balance from time to time and find it difficult to hold or lift objects.
Sometimes, an affected individual can have herniated discs without feeling any of the symptoms. In these cases, the only way to confirm is through imaging scans.
There are two major potential causes of disc herniation.
The entire body is designed to move together. When one part of the body stops moving other parts have to move more. When the spine moves more than its designed to move the disc material can rupture or tear. The most common areas that lack motion in the body are the hips and upper spine, when those areas have decreased motion the disc moves more and can herniate.
Trauma is another leading cause of disc herniation. When the spinal discs are naturally weakened by disc degeneration, additional intense stress can push them over the edge. This can happen when a person tries to lift something heavy using their back instead of their leg and thigh muscles.
A sudden twist or flex can also shock the discs enough to rupture. Other high-impact traumas such as a fall or an accident can lead to herniated discs in the spinal column as well.
Obesity also increases the risk of disc herniation because of the additional stress weight contributes.
Learn more about disc herniation by visiting the Mayo Clinic.
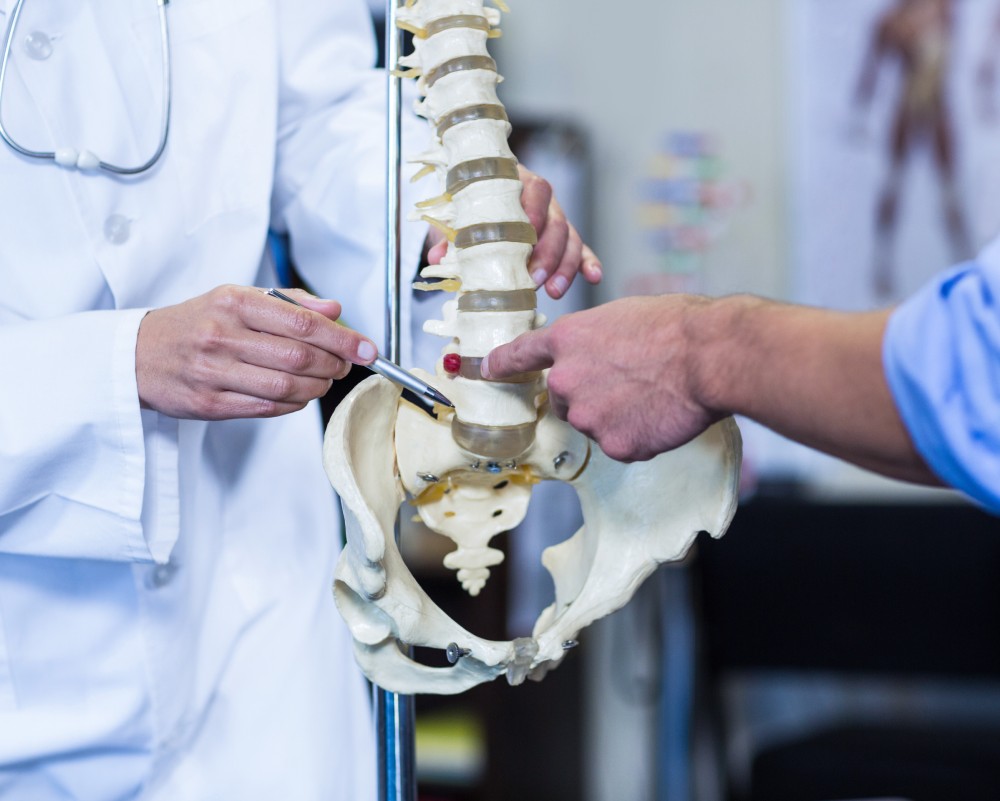
Once the doctor determines from the symptoms that the problem may be disc herniation, they will conduct a physical examination to identify the extent of the issue. The exam may include the following:
A neurological exam is done to check the muscle strength in the leg or arm, to detect whether there is loss of sensation, and to test the reflexes in the affected areas.
For disc herniation in the lower back, a straight leg raise or SLR test is done to confirm disc herniation for patients under 35.
Imaging scans may also be conducted for a clearer view of the issue.
MRI is used to see the body’s soft tissues, which include the spinal discs. It can also determine whether spinal nerves are affected. An MRI should not be done unless there are red flag symptoms that indicate surgery may be neccesary such as loss of control of bowl or bladder function, or muscle strength loss in the effected extermity. Otherwise MRI's lead to unecessary procedures for back pain that do not resolve the problem.
There are both non-surgical and surgical options for treating herniated discs. Doctors often recommend the following:
Rest – Doctors may suggest maintaining a low level of physical activity from a few days to several weeks as the inflammation decreases naturally.
Medication – Nonsteroidal anti-inflammatory medication may also be recommended to help reduce swelling and pain.
Injection – Doctors may also recommend an epidural steroid injection straight into the exact location of the disc herniation in the spine. This procedure is guided by x-ray.
Surgery – If more conservative treatment options do not offer relief, doctors may offer surgical options that can relieve pressure, remove or replace the herniated disc, or permanently fuse two vertebrae together.

That said, there is no guarantee that these traditional treatment options will work. In fact, they have been found to work only 45% of the time. This is because their objective is just to relieve the pain and not address the underlying cause.
Our treatment options are different. They are designed to get to the bottom of the pain source and develop lasting relief.
The most important element of healing is identifying the cause. The cause is a movement disorder somewhere else in the body that is creating more stress in the injured area than the tissue can handle. A full body movement assessment is the most important aspect in finding the true cause. This involves assessing how mobile and stable the areas above and below the injured tissues are. Once the dysfunctional areas are identified the physical therapist can then prescribe home treatments to fix the problem areas.
In order to improve motion in the dysfunctional areas that are causing the increased stress on the painful injured tissues the most effect way to make a change in the body is to have a physical therapist use their hands to facilitate the proper motion while you are moving at the same time. This helps improve the path the body takes in order to reduce stress and tenson on the injured area.
Through a series of curated exercises, pain and the symptoms are migrated into the middle line of the body where it is addressed until completely eliminated. This method can reduce pain immediately while enhancing function in the long-term.
In order to know which treatment option is best for you, get into an easy 15-min call with our Dr. Andrew Gorecki. In the last 15 years, he has been helping patients find lasting relief from their persistent pains through his very own “Superior Method.”
Find out more about this method and the more effective treatment options we offer during your free consultation. Call 231.944.6541 or email info@thesuperiortherapy.com to get lasting relief from your herniated disc.
Back pain injections, such as epidural injections or nerve blocks, can be safe if done by a trained medical professional. However, as with any medical procedure, there is always a risk of side effects and complications, such as infection or nerve damage. Your doctor will be able to advise you on the risks and benefits of back pain injections and help you make an informed decision.
Back pain is a common symptom during pregnancy, and can be caused by a number of factors, including hormonal changes, weight gain, and the increased pressure on the spine from the growing uterus. Mild to moderate back pain can often be managed with simple self-care measures, such as exercises, heat therapy, and good posture. Severe or persistent back pain should be evaluated by a doctor to rule out more serious conditions.
Back pain and stomach pain can be related in some cases, for example, if the back pain is caused by a condition affecting the abdomen, such as a kidney stone or a bladder infection. However, it's important to seek medical attention to determine the cause of the symptoms, as they may be caused by a serious condition.
Back pain during contractions can occur during labor and delivery, as the uterus contracts and puts pressure on the lower back. Some women also experience back pain during early labor, as the baby's head begins to engage in the pelvis.
Back pain and chest pain can be related in some cases, such as if the back pain is caused by an injury to the chest or rib cage. However, chest pain can also be a symptom of serious conditions, such as heart attack or lung problems, so it's important to seek medical attention to rule out these possibilities.
Back pain is not usually a sign of pregnancy, and there are many other symptoms that are more commonly associated with pregnancy, such as missed periods, nausea, and fatigue. If you think you might be pregnant, it's important to take a pregnancy test and see your doctor for confirmation.
Back pain and constipation can be related in some cases, as the increased pressure on the abdominal muscles from constipation can cause pain in the lower back. Treatment for constipation can help relieve the back pain.
Back pain can be a symptom of pregnancy, but it's not always the case. Other common symptoms of pregnancy include missed periods, nausea, fatigue, and breast tenderness. If you're experiencing back pain and think you might be pregnant, it's important to see your doctor for confirmation.
Yes, back pain can cause chest pain, especially if the pain is caused by an injury or condition affecting the chest or rib cage. If you're experiencing chest pain along with back pain, it's important to seek medical attention to determine the cause.
Yes, back pain can cause nausea, as the pain can interfere with normal digestive function and trigger feelings of nausea. If you're experiencing back pain and nausea, it's important to seek medical attention to determine the cause.
Yes, back pain can cause stomach pain, especially if the pain is caused by a condition affecting the abdomen, such as a kidney stone or a bladder infection. If you're experiencing both back pain and stomach pain, it's important to seek medical attention to determine the cause.
Yes, back pain can cause headaches, as the pain and stress can trigger tension headaches or migraines. If you're experiencing both back pain and headaches, it's important to seek medical attention to determine the cause and get appropriate treatment.
No, back pain is not a reliable sign of pregnancy. There are many other symptoms that are more commonly associated with pregnancy, such as
While back pain itself does not directly cause high blood pressure, the stress and anxiety that can accompany chronic pain can contribute to the development of high blood pressure. It is important to manage both conditions effectively to improve overall health.
In some cases, back pain can be a symptom of a more serious underlying condition such as cancer, especially when it is accompanied by other symptoms such as weight loss, fatigue, or fever. However, it is important to note that most cases of back pain are caused by non-cancerous conditions such as muscle strain or injury.
Back pain can occur due to a variety of reasons such as injury, overuse, aging, arthritis, a herniated disc, or conditions affecting the bones, muscles, or nerves in the back. It can also be a result of poor posture, sedentary lifestyle, or a combination of factors.
Back pain can happen as a result of physical strain, injury, or a condition that affects the bones, muscles, or nerves in the back. This can include activities such as heavy lifting, repetitive motions, or prolonged sitting, as well as underlying conditions such as arthritis, spinal stenosis, or osteoporosis.
The best course of treatment for back pain will depend on the underlying cause. Common options include over-the-counter pain medication, physical therapy, heat therapy, massage, chiropractic care, and in some cases, surgery. In addition, lifestyle changes such as maintaining proper posture, engaging in regular exercise, and maintaining a healthy weight can also help alleviate back pain and prevent it from recurring.
Back pain can have a significant impact on daily activities and quality of life. It can limit mobility, cause difficulty with work or personal tasks such as standing, sitting, or walking for prolonged periods, and contribute to stress and anxiety. Chronic back pain can also lead to depression and decreased physical and emotional well-being.
Back pain relief options vary, but common remedies include pain medication, physical therapy, hot or cold therapy, exercise, massage, chiropractic care, and in some cases, surgery. In addition, lifestyle changes such as maintaining proper posture, engaging in regular exercise, and maintaining a healthy weight can also help alleviate back pain and prevent it from recurring.
Back pain can have a significant impact on daily activities and quality of life. It can limit mobility, cause difficulty with work or personal tasks, and contribute to stress and anxiety. Chronic back pain can also lead to depression and decreased physical and emotional well-being. In addition, it can make it difficult to participate in leisure activities and maintain relationships, leading to decreased overall satisfaction with life.
It is difficult to determine the specific type of back pain without a thorough evaluation by a medical professional. A doctor may use various diagnostic tests, including X-rays, MRI, and physical examination, to determine the cause of the pain.
Back pain can be caused by a variety of factors, including injury, overuse, aging, arthritis, a herniated disc, or conditions affecting the bones, muscles, or nerves in the back. It can also be a result of poor posture, sedentary lifestyle, or a combination of factors.
Back pain can feel like a dull ache, sharp stabbing pain, or a burning sensation, depending on the cause. The location and intensity of the pain can also vary, and it may be accompanied by muscle spasms, stiffness, or tenderness.
Back pain refers to discomfort, soreness, or ache in the lower or upper back region.
The severity and frequency of back pain required for disability benefits vary and depend on several factors, such as the type of work, medical conditions, and overall health. A doctor can evaluate if back pain qualifies for disability.
A diagnosis of the specific type of back pain can only be determined by a medical professional after a thorough evaluation, including a physical examination and possibly imaging tests.
Severe or worsening back pain, accompanied by symptoms like fever, numbness, tingling, or loss of bladder or bowel control, can indicate a serious underlying medical condition and should be promptly evaluated by a doctor.
Back pain can cause referred pain in other areas of the body, including the chest. This is because the nerves that serve the back also serve other regions. Chest pain should be evaluated by a doctor to determine the underlying cause.
Back pain is a common complaint during pregnancy due to the changes in weight distribution and increased stress on the lower back. It can be treated with simple measures such as rest, exercise, and proper posture.
Back pain can cause referred pain or radiculopathy (nerve pain) in the legs. This occurs when a nerve in the back is compressed or irritated.
Mild to moderate low back pain is common during pregnancy and usually improves with rest, exercise, and proper posture. However, if the pain is severe or persistent, a doctor should be consulted.
Back pain is a common issue that refers to discomfort or pain in the lower, middle, or upper back. It can be caused by a variety of factors including injury, strain, or underlying medical conditions.
Back pain that is so severe and persistent that it significantly limits a person's ability to perform essential daily activities and work may qualify for disability benefits.
Back pain can be considered serious if it is accompanied by other symptoms such as fever, weakness in the legs, loss of bladder or bowel control, or unexplained weight loss. In such cases, prompt medical attention is necessary.
Chest pain along with back pain can be a sign of various conditions, including heart disease, lung problems, and muscular or nerve issues. It is important to seek medical attention immediately if this type of pain is experienced.
Back pain during pregnancy is common due to the changes in a woman's posture and weight as the baby grows. Hormonal changes and pressure on the lower back from the growing uterus can also contribute to back pain during pregnancy.
Leg pain in addition to back pain can be a sign of various conditions, including sciatica, nerve compression, or spinal stenosis. In some cases, the cause may be related to the back, while in others it may be due to a separate issue in the legs.
Mild to moderate back pain during pregnancy is considered normal as a result of the physical changes and increased weight. However, it is important to speak with a healthcare provider if the pain becomes severe or persistent.
Back pain can be a symptom of a serious underlying condition, such as a spinal cord injury, nerve damage, or a serious infection. Severe or worsening back pain, accompanied by symptoms like fever, numbness, tingling, or loss of bladder or bowel control, should be promptly evaluated by a doctor.
Back pain can be a symptom of spinal cancer, but it is not always an indicator. A doctor should be consulted to determine the underlying cause of the back pain.
Severe or persistent back pain during pregnancy, especially accompanied by other symptoms like abdominal pain or vaginal bleeding, can indicate a complication and should be evaluated by a doctor.
Back pain can be considered too much if it interferes with daily activities and quality of life, or if it is severe and persistent. A doctor should be consulted to determine the underlying cause and appropriate treatment.
Back pain that moves from side to side may indicate a more serious underlying condition and should be evaluated by a doctor.
Back pain can cause referred pain in other areas of the body, including the abdomen, which can cause nausea. A doctor should be consulted to determine the underlying cause.
Back pain can be caused by many factors, including muscular strain, nerve irritation, or a more serious underlying medical condition. A doctor should be consulted to determine the cause of the back pain.
Back pain can get worse with prolonged sitting or standing, improper posture, heavy lifting, or other physical activities. It can also worsen with age or underlying medical conditions. A doctor should be consulted to determine the underlying cause and appropriate treatment.
Back pain is considered serious if it is accompanied by other symptoms such as fever, weakness in the legs, loss of bladder or bowel control, or unexplained weight loss. Prompt medical attention is necessary in such cases.
Back pain can be a symptom of cancer, but it is not always a definitive sign. Cancer-related back pain is usually accompanied by other symptoms such as weight loss, fatigue, and weakness. A doctor should be consulted if back pain persists or is accompanied by other symptoms.
Back pain during pregnancy should be concerning if it is severe, persistent, or accompanied by other symptoms such as vaginal bleeding or decreased fetal movement. In such cases, prompt medical attention is necessary.
Back pain is considered too much when it interferes with a person's daily activities and causes significant discomfort. If back pain is persistent or becomes more severe, a doctor should be consulted.
It is concerning if back pain moves from side to side as this may indicate a more serious underlying condition. If this type of pain is experienced, a doctor should be consulted for a proper evaluation.
Back pain during periods can be caused by various factors such as hormonal changes, muscle cramps, and changes in posture. The hormonal changes during menstrual cycles can cause inflammation and pain in the lower back.
Back pain is a common symptom of COVID-19, especially in severe cases. The reason behind it is still unknown but it could be related to the inflammation and pressure on the chest caused by the virus.
Back pain is a common experience during pregnancy as the body adjusts to the growing uterus, changes in posture, and weight gain. Hormonal changes during pregnancy can also cause ligaments to loosen and lead to back pain.
Back pain before periods can be a result of hormonal changes and muscle tension caused by PMS (premenstrual syndrome).
Back pain when sick can be caused by various reasons such as coughing, sneezing, or lying down for long periods. Also, some illnesses such as the flu or pneumonia can cause inflammation and pain in the back.
Back pain that comes and goes can be caused by various factors such as posture, lifestyle, physical activity, and certain medical conditions. Sometimes, back pain can be the result of an injury or strain that takes time to heal.
Back pain after an epidural can be caused by the insertion of the needle or due to nerve irritation. Some people may also experience soreness in the lower back from lying in one position for a long time during labor.
Back pain in early pregnancy can be caused by various factors such as hormonal changes, increased weight, and changes in posture. As the uterus expands and the body adjusts, the weight shift can cause lower back pain.
Back pain can go away, however, the timeline depends on the underlying cause and severity of the pain. Simple back pain can go away with proper treatment and self-care, while chronic back pain may require more comprehensive treatment and a longer recovery time.
In some cases, back pain can go away on its own with proper self-care and adequate rest. However, if the pain persists or becomes severe, it's best to seek medical attention to determine the underlying cause and find the appropriate treatment.
Back pain can go away, but the timeline for recovery depends on the underlying cause and severity of the pain. Chronic back pain may require long-term treatment and management, but with proper care, most people can experience a significant reduction in pain.
Back pain itself doesn't directly cause high blood pressure, but certain underlying conditions such as kidney problems, infection, or spinal issues can cause both back pain and high blood pressure.
Back pain can cause nausea in some individuals as a result of muscle tension, inflammation, or nerve irritation. In severe cases, underlying medical conditions such as a herniated disc or spinal stenosis can cause nausea and back pain.
Back pain from an epidural can go away, but the timeline for recovery depends on the individual and the severity of the pain. Some people may experience soreness and discomfort for a few days, while others may experience more significant pain that takes longer to subside.
Back pain can cause chest pain in some individuals, especially
